Abstract
1076
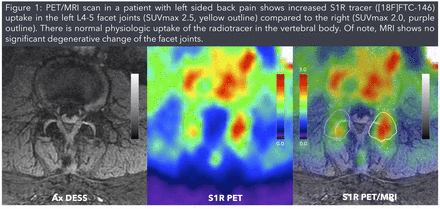
Objectives: The sigma-1 receptor (S1R) has been found to be an important modulator of signaling mechanisms in pain and inflammation, and its expression is upregulated at regions of heightened nociception in the periphery. Indeed, whole body [18F]FTC-146 PET/MRI, a highly selective PET (positron emission tomography) radioligand for the S1R, has shown increased uptake at sites of pain generation (for example, in Fig. 1). The purpose of this study is to determine whether [18F]FTC-146 shows differential binding in the brain of chronic pain patients compared to asymptomatic volunteers. Results from this study will potentially help determine whether expression of S1R in the brain plays a role in pain perception and central sensitization, and may also support the development of S1R-specific drugs for treating pain.
Methods: Healthy asymptomatic volunteers (4 female, 2 male) and pain patients (3 female, 2 male) experiencing low back and pelvic pain were recruited and written informed consent was received from each. The pain intensity of patients was reported as a minimum of 4 out of 10 on a numerical pain scale, for no less than 6 months. A GE SIGNA PET/MRI system (time-of-flight PET; 3.0T MRI bore) was used for the whole-body PET/MRI scans consisting of eight to ten stations. The injection dose of [18F]FTC-146 was 10 mCi, and imaging of the brain began immediately after intravenous injection while imaging of whole-body (head-to-toe) began 40 minutes after injection. Corresponding static PET images and MRI scans were matched, normalized and referenced to the white matter region in PMOD 3.7 (PMOD Technologies LLC). Average SUV and standard deviation were collected. We performed an unpaired t-test to determine the significance of the SUV in detected lesions in comparison with the corresponding measurements from healthy volunteers.
Results: Eighty-three predetermined VOIs (volumes of interest) were collected using the segmented adult brain MRI atlas in PMOD. Visual display showed that the precentral gyrus, hippocampus, amygdala, thalamus, and insula exhibited a significantly greater uptake of [18F]FTC-146 when graphed against healthy controls. The mean and standard deviation of SUV from patients in the precentral gyrus / hippocampus / amygdala / cuneus / thalamus / insula were 1.75 ± 1.01 (p<0.0024)/ 1.28 ± 0.59 (p<0.097) / 1.15 ± 0.54 (p<0.073) / 1.73 ± 0.91 (p<0.007)/ 1.56 ± 0.74 (p<0.085)/ 1.47 ± 0.86 (p<0.01), while those for the healthy volunteers were 1.47 ± 0.70 / 1.19 ± 0.65 / 1.05 ± 0.48 / 1.49 ± 0.56 / 1.50 ± 0.45 / 1.39 ± 0.63, respectively. In Figure 2, a greater uptake in the right side of the thalamus can possibly be attributed to the patient’s low back and left leg pain.
Conclusions: Sigma-1 receptor shows significantly (p<0.05) increased S1R radiotracer binding in precentral gyrus, cuneus, and insula; components of the brain ‘pain matrix’, which is a collection of neural centers involved in both physiological and cognitive/emotional aspects of pain processing. While more homogeneous patient samples, with respect to pain classification and participant differences would reduce variability, there appears to be a significant relationship between one’s experience with pain and sigma-1 receptor binding. Future studies are planned to determine whether S1R binding patterns correlate with location of and intensity of pain and also help predict if an individual may be refractory to certain treatments.