Abstract
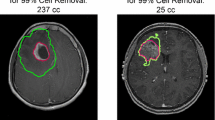
Microscopic invasion of tumor cells and undetected tumor proliferation is the primary reason for a dismal prognosis in glioblastoma patients. Identification and quantification of spatially localized brain regions undergoing high rates of cell migration and proliferation is critical for improving patient survival; however, there are currently no non-invasive imaging biomarkers for estimating proliferation and migration rates of human gliomas in vivo. To accomplish this, we developed CIMPLE (cell invasion, motility, and proliferation level estimates) image maps using serial diffusion MRI scans and a solution to a glioma growth model equation. CIMPLE represent a novel method of quantifying the level of aggressive malignant behavior. In the current pilot study, we demonstrate the utility of CIMPLE maps to predict progression free survival (PFS) and overall survival (OS) in 26 recurrent glioblastoma patients treated with bevacizumab from our Neuro-Oncology database. Voxel-wise estimates of cell proliferation rate predicted spatial regions of contrast enhancement in 35% of patients. A linear correlation was found between the mean proliferation rate and progression-free survival (PFS; P < 0.0001) as well as overall survival (OS; P = 0.0093). Similarly, the mean proliferation rate was able to stratify patients with early and late PFS as well as OS.




Similar content being viewed by others
References
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ, Belanger K, Brandes AA, Morosi C, Bogdahn U, Curschmann J, Janzer RC, Ludwin SK, Gorlia T, Allgeier A, Lacombe D, Cairncross JG, Eisenhauer E, Mirimanoff RO (2005) Radiotherapy plus concomitant and adjuvent temozolomide for glioblastoma. N Engl J Med 352:987–996
Murakami M, Jay V, Al-Shail E, Rutka JT: Brain tumors that disseminate along cerebrospinal fluid pathways and beyond (1998) In: Mikkelsen T, Bjerkvig R, Laerum OD, Rosenblum ML (eds) Brain tumor invasion: biological, clinical and therapeutic considerations. Wiley-Liss, Inc., New York, pp 111–132
Ellingson BM, Rand SD, Malkin MG, Prost R, Connelly JM, LaViolette PS, Bedekar DP, Schmainda KM (2010) Spatially quantifying microscopic tumor invasion and proliferation using a voxel-wise analytical solution to a glioma growth model and serial diffusion MRI. Proc Intl Soc Mag Reson Med 18:612
Ellingson BM, LaViolette PS, Rand SD, Malkin MG, Connelly JM, Mueller WM, Prost RW, Schmainda KM (2011) Spatially quantifying microscopic tumor invasion and proliferation using a voxel-wise solution to a glioma growth model and serial diffusion MRI. Magn Reson Med 65(4):1131–1143
Ellingson BM, Malkin MG, Rand SD, Connelly JM, Quinsey C, LaViolette PS, Bedekar DP, Schmainda KM (2010) Validation of functional diffusion maps (fDMs) as a biomarker for human glioma cellularity. J Magn Reson Imaging 31:538–548
Rockne R, Alvord EC Jr, Rockhill JK, Swanson KR (2009) A mathematical model for brain tumor response to radiation therapy. J Math Biol 58:561–578
Swanson KR, Rostomily RC, Alvord EC Jr (2008) A mathematical modelling tool for predicting survival of individual patients following resection of glioblastoma: a proof or principle. Br J Cancer 98:113–119
Swanson KR, Alvord EC Jr, Murray JD (2002) Quantifying efficacy of chemotherapy of brain tumors with homogeneous and heterogeneous drug delivery. Acta Biotheor 50:223–237
Reese TG, Heid O, Weisskoff RM, Wedeen VJ (2003) Reduction of eddy-current-induced distortion in diffusion MRI using a twice-refocused spin echo. Magn Reson Med 49:177–182
Macdonald DR, Cascino TL, Schold SC Jr, Cairncross JG (1990) Response criteria for phase II studies of supratentorial malignant glioma. J Clin Oncol 8:1277–1280
Pope WB, Sayre J, Perlina A, Villablanca JP, Mischel PS, Cloughesy TF (2005) MR imaging correlates of survival in patients with high-grade gliomas. AJNR Am J Neuroradiol 26:2466–2474
Farlow SJ (1993) Partial differential equations for scientists and engineers. Wiley, New York
Cox RW, Jesmanowicz A (1999) Real-time 3D image registration for functional MRI. Magn Reson Med 42:1014–1018
Nghiemphu PL, Liu W, Lee Y, Than T, Graham C, Lai A, Green RM, Pope WB, Liau LM, Mischel PS, Nelson SF, Elashoff R, Cloughesy TF (2009) Bevacizumab and chemotherapy for recurrent glioblastoma: a single-institution experience. Neurology 72:1217–1222
Vredenburgh JJ, Desjardins A, Herndon JE, Dowell JM, Reardon DA, Quinn JA, Rich JN, Sathornsumetee S, Gururangan S, Wagner M, Bigner DD, Friedman AH, Friedman HS (2007) Phase II trial of bevacizumab and irinotecan in recurrent malignant glioma. Clin Cancer Res 13:1253–1259
Friedman AH, Prados MD, Wen PY, Mikkelsen T, Schiff D, Abrey LE, Yung WK, Paleologos N, Nicholas MK, Jensen R, Vredenburgh J, Huang J, Zheng M, Cloughesy T (2009) Bevacizumab alone and in combination with irinotecan in recurrent glioblastoma. J Clin Oncol 27:4733–4740
Iwamoto FM, Abrey LE, Beal K, Gutin PH, Rosenblum ML, Reuter VE, DeAngelis LM, Lassman AB (2009) Patterns of relapse and prognosis after bevacizumab failure in recurrent glioblastoma. Neurology 73:1200–1206
Norden AD, Young GS, Setayesh K, Muzikansky A, Klufas R, Ross GL, Ciampa AS, Ebbeling LG, Levy B, Drappatz J, Kesari S, Wen PY (2008) Bevacizumab for recurrent malignant gliomas: efficacy, toxicity, and patterns of recurrence. Neurology 70:779–787
Pope WB, Kim HJ, Huo J, Alger J, Brown MS, Gjertson D, Sai V, Young JR, Tekchandani L, Cloughesy TF, Mischel PS, Lai A, Nghiemphu PL, Rahmanuddin S, Goldin J (2009) Recurrent glioblastoma multiforme: ADC histogram analysis predicts response to bevacizumab treatment. Radiology 252:182–189
Ellingson BM, Malkin MG, Rand SD, LaViolette PS, Connelly JM, Mueller WM, Schmainda KM (2011) Volumetric analysis of functional diffusion maps (fDMs) is a predictive imaging biomarker for cytotoxic and anti-angiogenic treatments in malignant gliomas. J Neurooncol 102(1):95–103
Sorensen AG, Batchelor TT, Zhang WT, Chen PJ, Yeo P, Wang M, Jennings D, Wen PY, Lahdenranta J, Ancukiewicz M, di Tomaso E, Duda DG, Jain RK (2009) A “vascular normalization index” as potential mechanistic biomarker to predict survival after a single dose of cediranib in recurrent glioblastoma patients. Cancer Res 69:5296–5300
Chen W, Delaloye S, Silverman DH, Geist C, Czernin J, Sayre J, Satyamurthy N, Pope W, Lai A, Phelps ME, Cloughesy T (2007) Predicting treatment response of malignant gliomas to bevacizumab and irinotecan by imaging proliferation with [18F] fluorothymidine positron emission tomography: a pilot study. J Clin Oncol 25:4714–4721
Sawlani RN, Raizer J, Horowitz SW, Shin W, Grimm SA, Chandler JP, Levy R, Getch C, Carroll TJ (2010) Glioblastoma: a method for predicting response to antiangiogenic chemotherapy by using MR perfusion imaging—pilot study. Radiology 255:622–628
Kelly PJ, Daumas-Duport C, Scheithauer BW, Kall BA, Kispert DB (1987) Stereotactic histological correlations of computed tomography- and magnetic resonance imaging-defined abnormalities in patients with glial neoplasms. Mayo Clin Proc 62:450–459
Kelly PJ, Daumas-Duport C, Kispert DB, Kall BA, Scheithauer BW, Illig JJ (1987) Imaging-based stereotaxic serial biopsies in untreated intracranial glial neoplasms. J Neurosurg 66:865–874
Verhoeff JJ, van Tellingen O, Claes A, Stalpers LJ, van Linde ME, Richel DJ, Leenders WP, van Furth WR (2009) Concerns about anti-angiogenic treatment in patients with glioblastoma multiforme. BMC Cancer 9:444
Norden AD, Drappatz J, Wen PY (2009) Antiangiogenic therapies for high-grade glioma. Nat Rev Neurol 5:610–620
de Groot JF, Fuller G, Kumar AJ, Piao Y, Eterovic K, Ji Y, Conrad CA (2010) Tumor invasion after treatment of glioblastoma with bevacizumab: radiographic and pathologic correlation in humans and mice. Neuro Oncol 12:233–242
Swanson KR, Alvord EC Jr, Murray JD (2000) A quantitative model for differential motility of gliomas in grey and white matter. Cell Prolif 33:317–329
Harpold HLP, Alvord EC Jr, Swanson KR (2007) The evolution of mathematical modeling of glioma proliferation and invasion. J Neuropathol Exp Neurol 66:1–9
Lyng H, Haraldseth O, Rofstad EK (2000) Measurements of cell density and necrotic fraction in human melanoma xenografts by diffusion weighted magnetic resonance imaging. Magn Reson Med 43:828–836
Sugahara T, Korogi Y, Kochi M, Ikushima I, Shigematu Y, Hirai T, Okudo T, Liang L, Ge Y, Komohara Y, Ushio Y, Takahashi M (1999) Usefulness of diffusion-weighted MRI with echo-planar technique in the evaluation of cellularity in gliomas. J Magn Reson Imaging 9:53–60
Chenevert TL, Stegman LD, Taylor JM, Robertson PL, Greenberg HS, Rehemtulla A, Ross BD (2000) Diffusion magnetic resonance imaging: an early surrogate marker for therapeutic efficacy in brain tumors. J Natl Cancer Inst 92:2029–2036
Hayashida Y, Hirai T, Morishita S, Kitajima M, Murakami R, Korogi Y, Makino K, Nakamura H, Ikushima I, Yamura M, Kochi M, Kuratsu JI, Yamashita Y (2006) Diffusion-weighted imaging of metastatic brain tumors: comparison with histologic type and tumor cellularity. AJNR Am J Neuroradiol 27:1419–1425
Gauvain KM, McKinstry RC, Mukherjee P, Perry A, Neil JJ, Kaufman BA, Hayashi RJ (2001) Evaluating pediatric brain tumor cellularity with diffusion-tensor imaging. AJR Am J Roentgenol 177:449–454
Kinoshita M, Hashimoto N, Goto T, Kagawa N, Kishima H, Izumoto S, Tanaka H, Fujita N, Yoshimine T (2008) Fractional anisotropy and tumor cell density of the tumor core show positive correlation in diffusion tensor magnetic resonance imaging of malignant tumors. Neuroimage 43:29–35
Kono K, Inoue Y, Nakayama K, Shakudo M, Morino M, Ohata K, Wakasa K, Yamada R (2001) The role of diffusion-weighted imaging in patients with brain tumors. AJNR Am J Neuroradiol 22:1081–1088
Acknowledgments
This work was supported by Brain Tumor Funders Collaborative (WBP); Art of the Brain (TFC); Ziering Family Foundation in memory of Sigi Ziering (TFC); Singleton Family Foundation (TFC); Clarence Klein Fund for Neuro-Oncology (TFC).
Author information
Authors and Affiliations
Corresponding author
Appendix: Solution to the glioma growth equation using estimates of water mobility
Appendix: Solution to the glioma growth equation using estimates of water mobility
Using the glioma growth model developed by Swanson et al. [29, 30], we see the rate of change in glioma cell density is equal to the net invasion of glioma cells plus the net proliferation
where c is cell density, D is the diffusion coefficient of migrating cells, ρ is the cell proliferation rate, and t is time. Based on evidence of a strong negative correlation between tumor cell density and ADC of water measured using DWI [31–37], ADC can be substituted into Eq. 1 to yield
where ADC is the apparent diffusion coefficient of water as a three-dimensional scalar field (i.e. ADC image volume acquired using DWI), D is the diffusion coefficient of migrating cells as a three-dimensional scalar field, and ρ is the cell proliferation rate as a three-dimensional scalar field.
An analytical expression for cell diffusion rate, D, and proliferation rate, ρ, can be described by using the Methods of Characteristics [12] to achieve one possible solution:
and
where
describes the time-rate of change in ADC and
describes the ratio of ADC on the current day n with respect to the previous scan day n−1. Thus, using three ADC maps collected on days t n, t n−1, and t n−2, the proliferation rate, ρ, and cell motility (diffusion), D, can be directly estimated for the time interval spanned from t n−2 to t n using Eqs. 3–6. Analytical solutions to the glioma growth model were verified in Mathematica v7.01 (Wolfram Mathematica 7.01, Wolfram Research, Inc, Champaign, IL) and are further defined in a previous publication [4].
Rights and permissions
About this article
Cite this article
Ellingson, B.M., Cloughesy, T.F., Lai, A. et al. Cell invasion, motility, and proliferation level estimate (CIMPLE) maps derived from serial diffusion MR images in recurrent glioblastoma treated with bevacizumab. J Neurooncol 105, 91–101 (2011). https://doi.org/10.1007/s11060-011-0567-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-011-0567-8