Abstract
Purpose
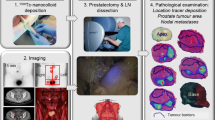
To present a modified concept for sentinel lymph node (SLN)-guided pelvic lymph node dissection in prostate cancer.
Methods
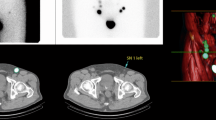
A total of 463 patients with histologically proven prostate cancer underwent SLN-guided lymph node dissection. The day before surgery patients received intraprostatic injection of Tc-99 m-labeled nanocolloid (Tc-NC) under transrectal ultrasound guidance. At the time of surgery, the lymph nodes of the obturator fossa were dissected routinely in all patients. After meticulous testing with a handheld gamma probe, all lymphatic tissues in predefined anatomic regions (external iliac, internal iliac, common iliacal and presacral) with Tc-NC uptake were additionally resected.
Results
In 146 (12.8%) patients, SLN were located exclusively in the obturator fossa, but 317 patients (87.2%) underwent resection of additional sentinel regions. In 28 (6.1%) patients, 62 lymph node metastases were detected, and 32 (51.6%) of these were located outside the obturator fossa. Eight (28.6%) patients displayed lymph node metastases exclusively outside the obturator fossa and had been resected only because of positive SLN probing.
Conclusions
The obturator fossa comprises the major landing site of lymph node metastases, but more than half of the metastases are located outside this anatomic region. Routine resection of the obturator fossa with additional resection of positive sentinel regions improves staging accuracy compared to resection of the obturator fossa only.


Similar content being viewed by others
References
Bader P, Burkhard FC, Markwalder R et al (2002) Is a limited lymph node dissection an adequate staging procedure for prostate cancer? J Urol 168:514–518
Briganti A, Blute ML, Eastham JH et al (2009) Pelvic lymph node dissection in prostate cancer. Eur Urol 55:1251–1265
Briganti A, Chun FK, Salonia A et al (2006) Complications and other surgical outcomes associated with extended pelvic lymphadenectomy in men with localized prostate cancer. Eur Urol 50:1006–1013
Cellini N, Luzi S, Mantini G et al (2003) Lymphatic drainage and CTV in carcinoma of the prostate. Rays 28:337–341
Cheng L, Zincke H, Blute ML et al (2001) Risk of prostate carcinoma death in patients with lymph node metastasis. Cancer 91:66–73
Clark T, Parekh DJ, Cookson MS et al (2003) Randomized prospective evaluation of extended versus limited lymph node dissection in patients with clinically localized prostate cancer. J Urol 169:145–147
Corvin S, Schilling D, Eichhorn K et al (2006) Laparoscopic sentinel lymph node dissection–a novel technique for the staging of prostate cancer. Eur Urol 49:280–285
Epstein JI, Partin AW, Sauvageot J et al (1996) Prediction of progression following radical prostatectomy. A multivariate analysis of 721 men with long-term follow-up. Am J Surg Pathol 20:286–292
Heidenreich A, Aus G, Bolla M et al (2008) EAU guidelines on prostate cancer. Eur Urol 53:68–80
Heidenreich A, Varga Z, Von Knobloch R (2002) Extended pelvic lymphadenectomy in patients undergoing radical prostatectomy: high incidence of lymph node metastasis. J Urol 167:1681–1686
Holl G, Dorn R, Wengenmair H et al (2009) Validation of sentinel lymph node dissection in prostate cancer: experience in more than 2, 000 patients. Eur J Nucl Med Mol Imaging 36:1377–1382
Hovels AM, Heesakkers RA, Adang EM et al (2008) The diagnostic accuracy of CT and MRI in the staging of pelvic lymph nodes in patients with prostate cancer: a meta-analysis. Clin Radiol 63:387–395
Hull GW, Rabbani F, Abbas F et al (2002) Cancer control with radical prostatectomy alone in 1, 000 consecutive patients. J Urol 167:528–534
Lam TK, Uren RF, Scolyer RA et al (2009) False-negative sentinel node biopsy because of obstruction of lymphatics by metastatic melanoma: the value of ultrasound in conjunction with preoperative lymphoscintigraphy. Melanoma Res 19:94–99
McLaughlin AP, Saltzstein SL, McCullough DL et al (1976) Prostatic carcinoma: incidence and location of unsuspected lymphatic metastases. J Urol 115:89–94
Stone NN, Stock RG, Unger P (1997) Laparoscopic pelvic lymph node dissection for prostate cancer: comparison of the extended and modified techniques. J Urol 158:1891–1894
Warncke SH, Mattei A, Fuechsel FG et al (2007) Detection rate and operating time required for gamma probe-guided sentinel lymph node resection after injection of technetium-99 m nanocolloid into the prostate with and without preoperative imaging. Eur Urol 52:126–132
Wawroschek F, Vogt H, Weckermann D et al (1999) The sentinel lymph node concept in prostate cancer—first results of gamma probe-guided sentinel lymph node identification. Eur Urol 36:595–600
Wawroschek F, Vogt H, Wengenmair H et al (2003) Prostate lymphoscintigraphy and radio-guided surgery for sentinel lymph node identification in prostate cancer. Technique and results of the first 350 cases. Urol Int 70:303–310
Weckermann D, Dorn R, Trefz M et al (2007) Sentinel lymph node dissection for prostate cancer: experience with more than 1, 000 patients. J Urol 177:916–920
Acknowledgments
The authors thank Miriam Germann for carefully reviewing and proof-reading the manuscript.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
David Schilling and Ulf Boekeler contributed equally.
Rights and permissions
About this article
Cite this article
Schilling, D., Boekeler, U., Gakis, G. et al. Modified concept for radioisotope-guided sentinel lymph node dissection in prostate cancer. World J Urol 28, 715–720 (2010). https://doi.org/10.1007/s00345-010-0533-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-010-0533-7